You're a physician who thinks you may have a process that you can patent?
You're a physician who thinks you may have a process that you can patent?
The US Patent law specifies 4 things that are patentable:
- Processes,
- Machines,
- Manufactures, and
- Compositions of matter.
When we think of patents most think of a gadget, which falls under the “machines” classification and is typically referred to as an “apparatus” when writing a patent. We will spend some time later on the apparatus patent but today will focus on the process patent.
First, a story to demonstrate the power of a process patent. In the 1950’s Monsanto produced the compound 3, 4-dichloropropionanilide and secured a patent on this compound. This compound is referred to as “propanil” which is obviously unrelated to the beta-blocker propanolol. In the late 1950’s Rohm & Haas found out that propanil was an excellent herbicide for rice. Monsanto filed suit against Rohm & Haas for patent infringement but the R&H lawyers found a paper from 1902 describing the compound and thus the patent was found invalid.
Note: this was all before the age of Internet search. Nowadays, there is no excuse for spending the money on a patent before an exhaustive (and largely free) search is done for what is called “prior art” in the patent lexicon.
Rohm & Haas then procured a process patent on a “method for applying propanil to inhibit the growth of undesirable plants in areas containing established crops.” Meanwhile Dawson Chemical was selling the compound so R&H sued them.
To the average person, this lawsuit must have seemed ridiculous. After all, R&H did not invent the compound nor were they the first to try to patent it. And, they were just lucky to find out that it was good with rice. What kind of breakthrough was that? Monsanto was long in the seed and herbicide business so clearly they must have thought that this compound could be used as an herbicide. Finally, Dawson was not actually applying the compound to the rice fields — it was the farmers. So, why not sue each individual farmer?
The appeals court ruled against Rohm & Haas but the Supreme Court took up the case. In one of the classic 5-4 decisions, the Supreme Court reversed the appeals court and ruled that:
1. A “repurposing” of an existing compound was worthy of a patent. In an informative paragraph the majority wrote:
“It is, perhaps, noteworthy that holders of "new use" patents on chemical processes were among those designated to Congress as intended beneficiaries of the protection against contributory infringement that § 271 was designed to restore. We have been informed that the characteristics of practical chemical research are such that this form of patent protection is particularly important to inventors in that field. The number of chemicals either known to scientists or disclosed by existing research is vast. It grows constantly, as those engaging in "pure" research publish their discoveries. The number of these chemicals that have known uses of commercial or social value, in contrast, is small. Development of new uses for existing chemicals is thus a major component of practical chemical research.”
2. Dawson was guilty of “contributory” infringement as propanil was not a staple good nor was there another substantial use for it other than as an herbicide. While Dawson did not actually apply the chemical they contributed by selling it when they had to know that it would be used primarily as an herbicide.
The decision can be read at: http://www.law.uconn.edu/homes/swilf/ip/cases/dawson.htm
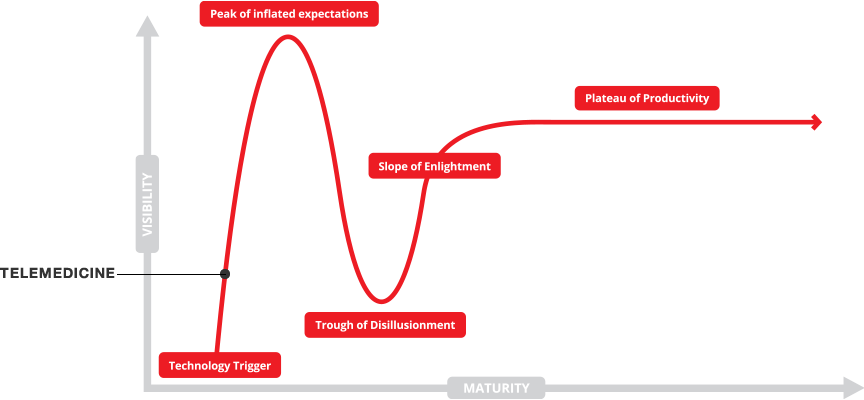
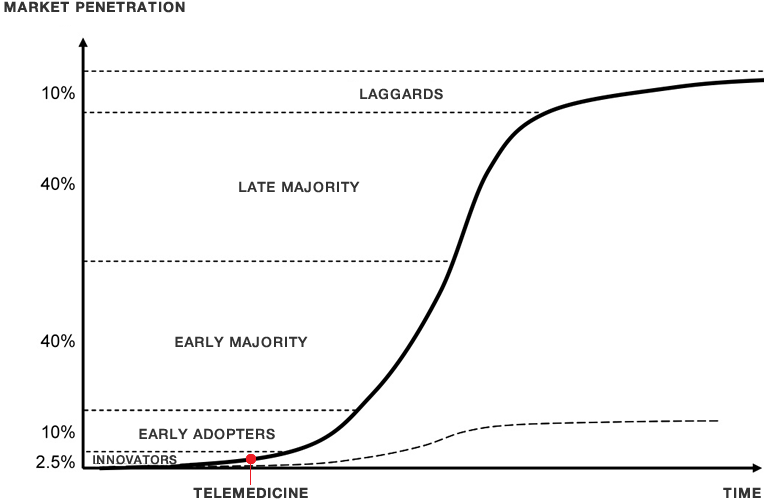
How does this apply to the physician inventor? Imagine that your were the first to notice that your patients on the diuretic diamox came back from their ski trips mentioning that they now had no problem with altitude sickness? You could get a patent on a process (typically now called a “method” patent) of preventing altitude sickness by taking diamox.
Fine. Now you have a patent. How do you enforce it? Do you sue every skier or mountaineer that takes it? No. However, if a drug manufacturer put that indication in its training or sales material then you could have grounds for a suit. Since this would require an FDA trial, the very study materials and FDA filings would be about all of the evidence that you would need. That alone might be enough for a drug company to approach you for a license. Especially after the off-label prescribing grew to the point that the drug company noticed it.
What could you do if the drug company is content with the off-label prescriptions? Not much unless the other indications (hypertension and glaucoma etc) amounted to a trivial portion of the prescriptions.





 Post a Comment
Post a Comment